29 Nov The hospital-at-home model–health care at your doorstep

The hospital-at-home model–health care at your doorstep
The effects of treatment and recovery in a hospital setting can seem like a cruel paradox. Admission to the hospital is often necessary for certain treatments; however, hospital stays can come with additional risks. It has long been known that hospitalization is associated with adverse outcomes, hospital-acquired infection, and mortality risk.1 Thus, many patients would prefer to receive treatment and recover in the comfort and safety of their own homes.
As a response to these risks, hospital-at-home (HaH) programs have been created to allow for necessary treatments for acute conditions to be done in patient homes. Such a model demonstrates a patient-centered approach to care and has been increasingly adopted in multiple fields of medicine. In fact, implementing at-home hospital services is one of the most extensively-researched reforms in health care, demonstrating safer, cheaper, and more effective care options for some acute conditions.2
The concept of HaH dates back to the 1970s when clinical trials in the United Kingdom determined that there were no specific benefits of hospitalization over home-based care for patients experiencing myocardial infarctions.3 Hospital-at-home programs have since been implemented in several countries, including the United Kingdom, Canada, Israel, and Australia.4 The United States has previously been slow to adopt HaH models of health care mainly due to hospitals having to fund these services independently.4
However, the COVID-19 pandemic required hospitals worldwide to adapt and use remote and digital health services. The recent emphasis on telehealth and digital health services has made monitoring and communicating with patients in at-home care settings easier than ever. Therefore, we have seen a rapid increase in the utilization of the HaH model in the United States. In response to the public health crisis caused by the pandemic, the Centers for Medicare & Medicaid Services (CMS) authorized the Acute Hospital Care at Home Waiver (AHCaH) in November 2020, establishing Medicare payment for at-home hospital care.5 The HaH model allowed patients suffering from certain non-COVID-19-related illnesses to be treated at home, reducing the risk of contracting the virus while clearing hospital beds to treat critical COVID-19 patients. During 2020 and 2021, 186 hospitals across 33 states applied for the CMS waiver to provide HaH services.6 In fact, hospitals continue to apply for the waiver.6
In 2021, prominent healthcare companies, including Kaiser Permanente, the Mayo Clinic, and Medically Home, banded together to form The Advanced Care at Home.7 This coalition’s mission is to support the advancement and adoption of HaH programs for healthcare systems around the country. Due to the positive outcome of the AHCaH program, a bipartisan bill (H.R. 7053 – Hospital Inpatient Services Modernization Act) has been drafted and aims to extend the CMS waiver program. In fact, physicians envision HaH care to be the new standard of care. John Hopkins’ Bruce Leff, MD, predicts, “One day, hospitals will be ERs, ORs, and ICUs. Everything else should get pushed out into the community.”8
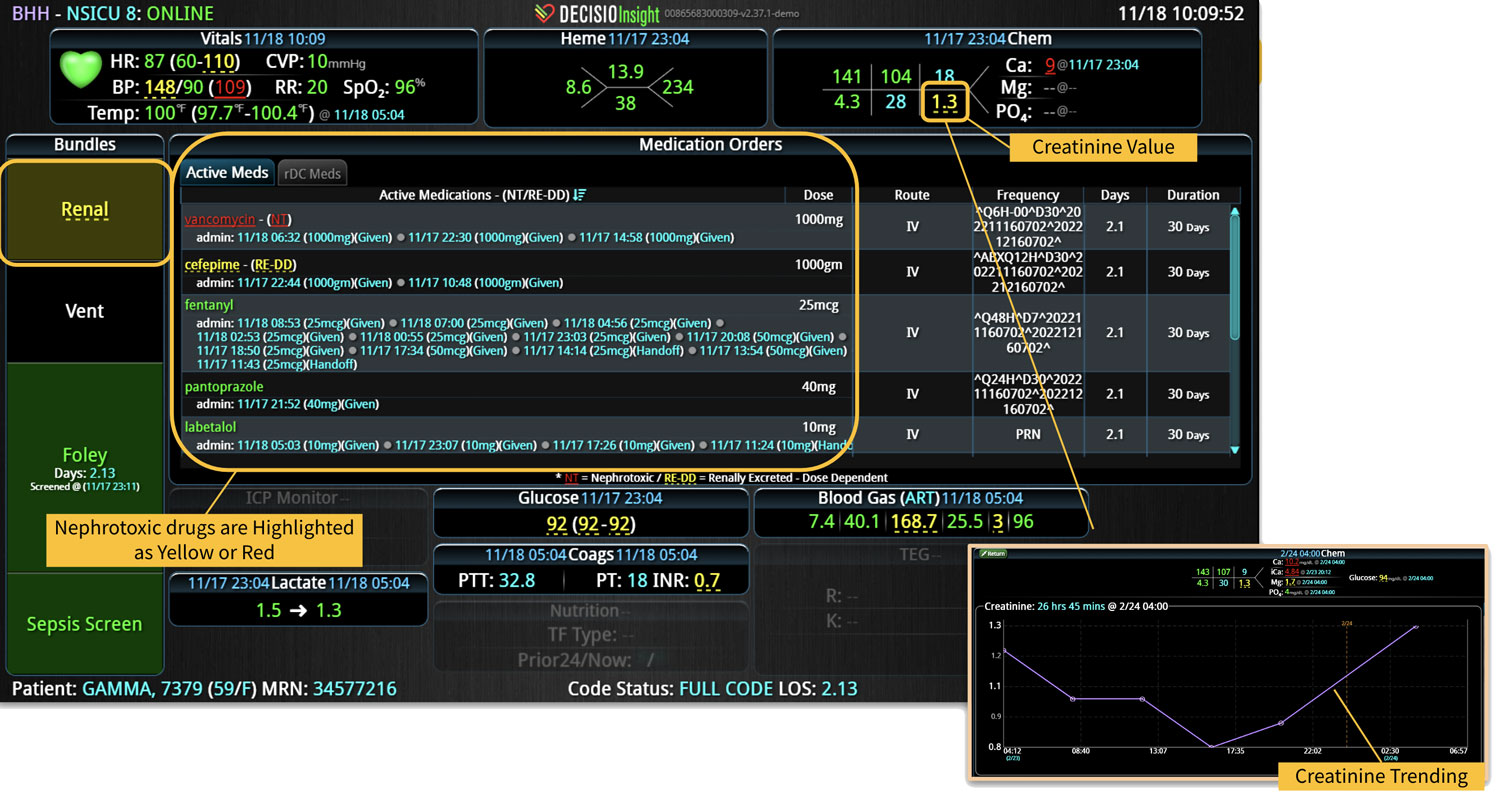
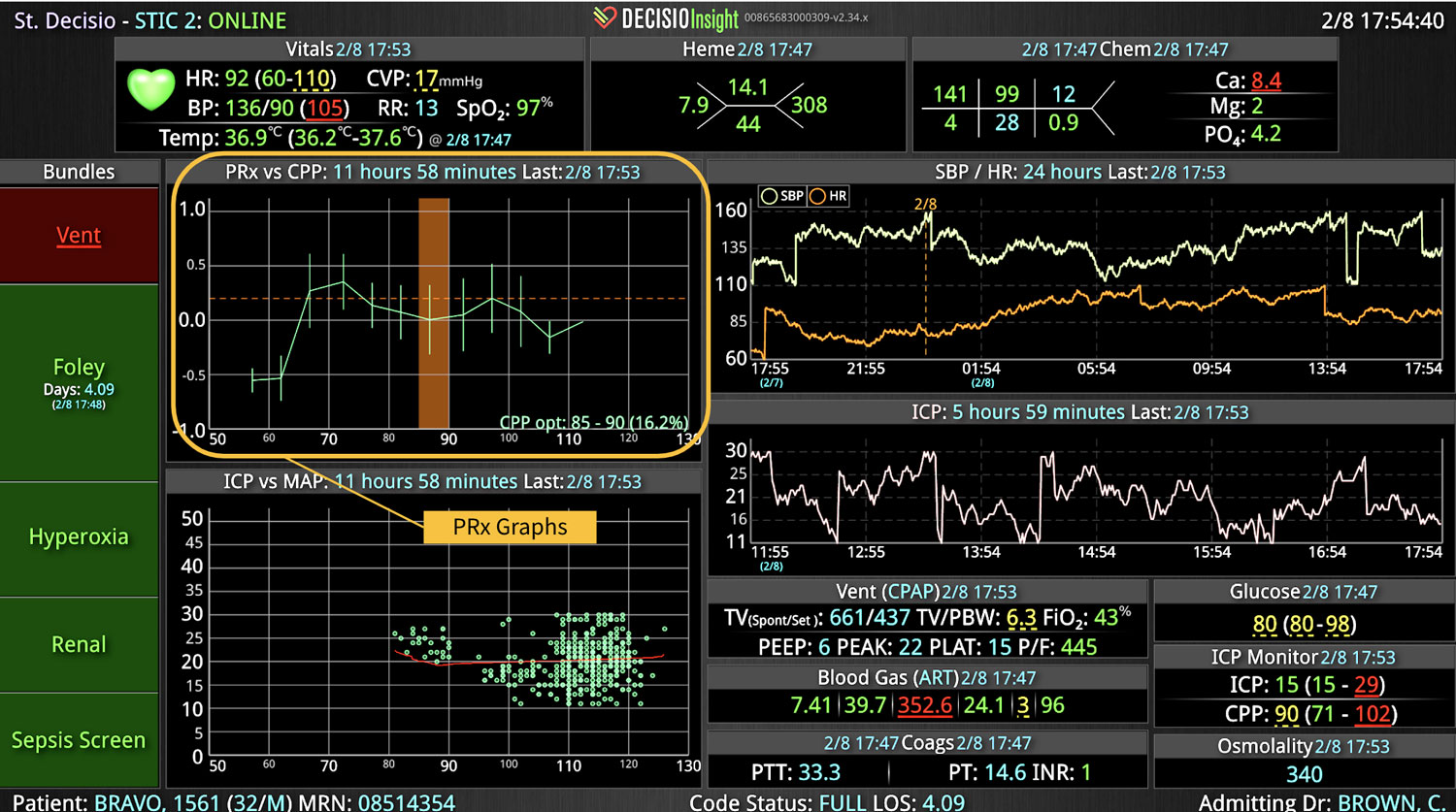
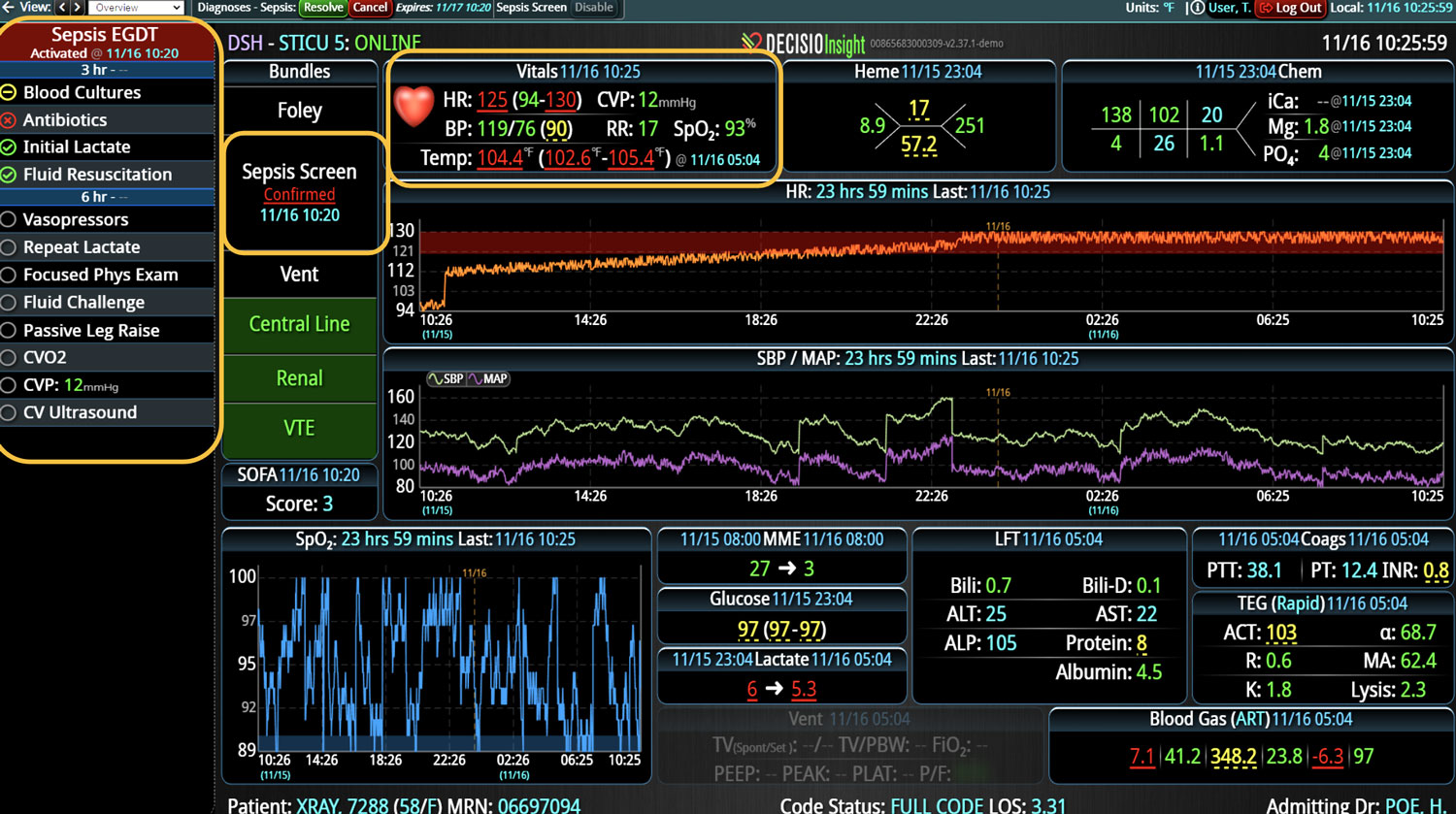
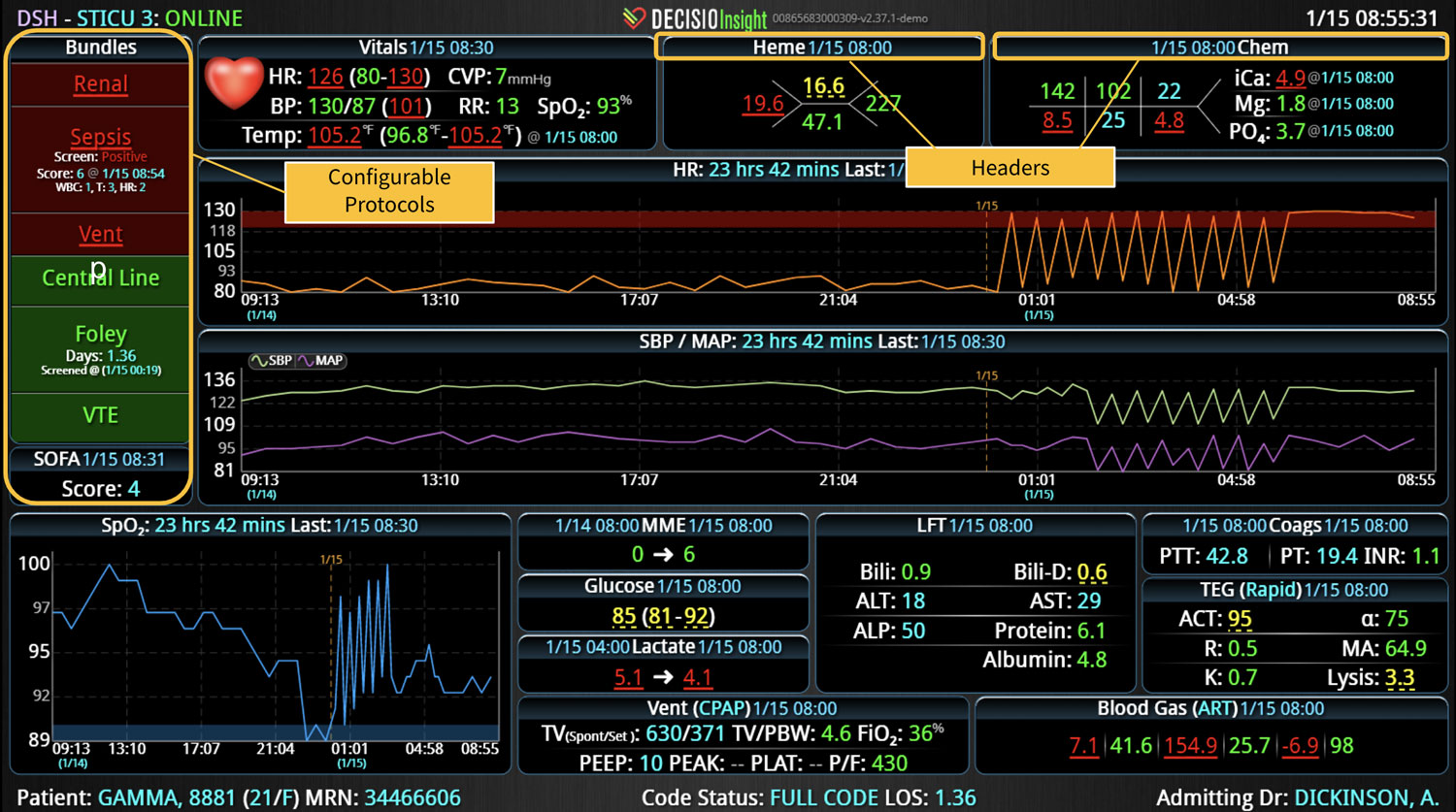
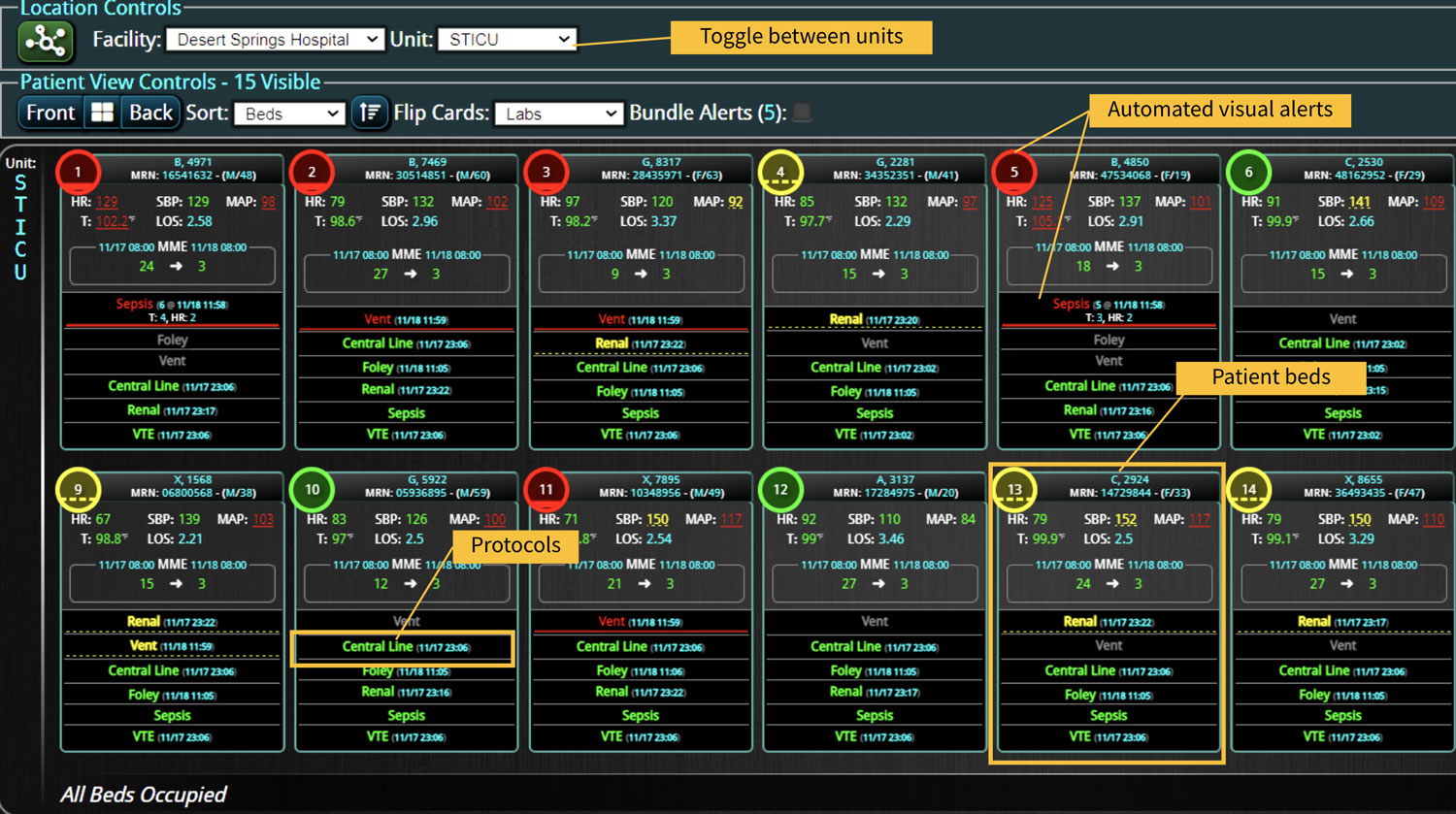
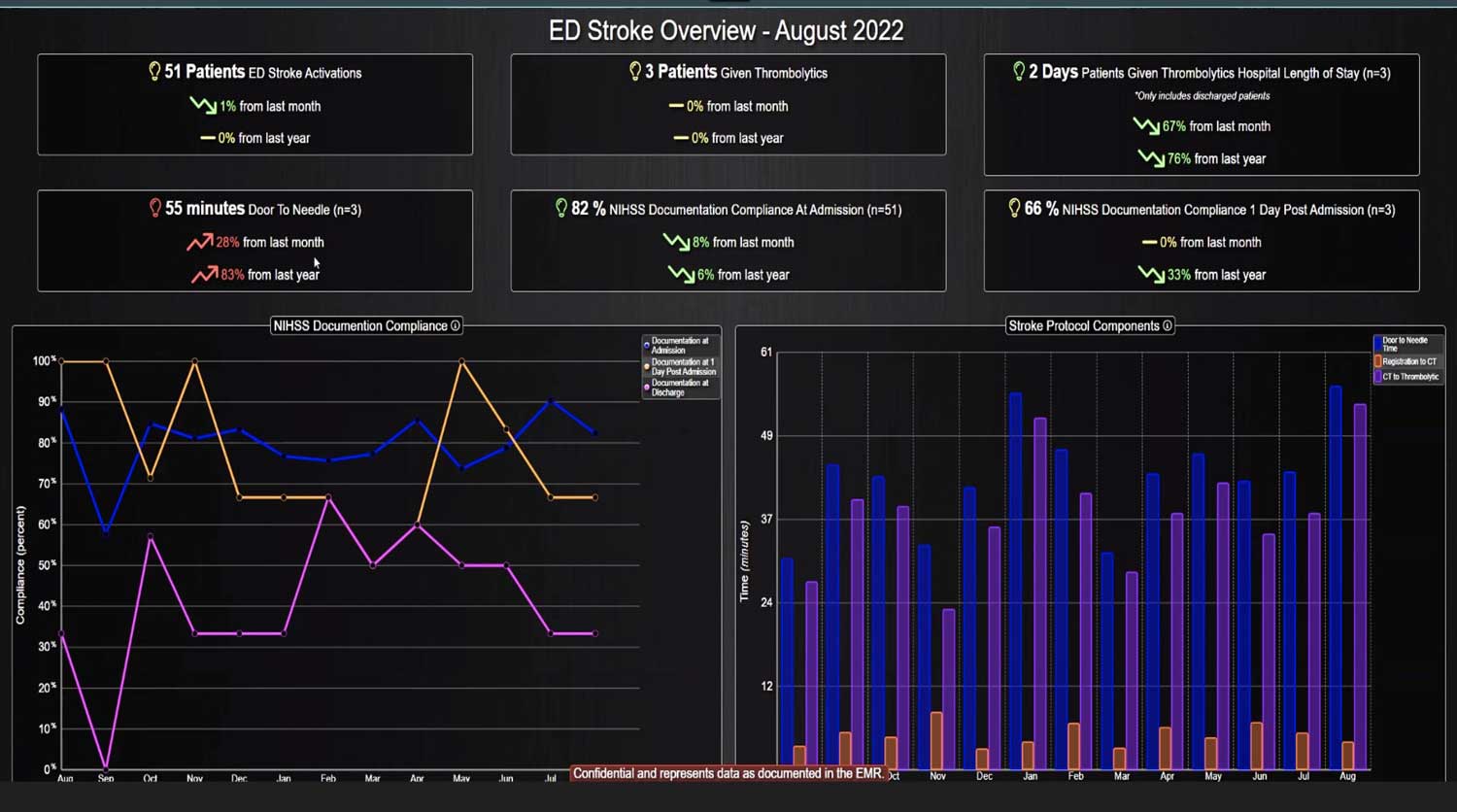
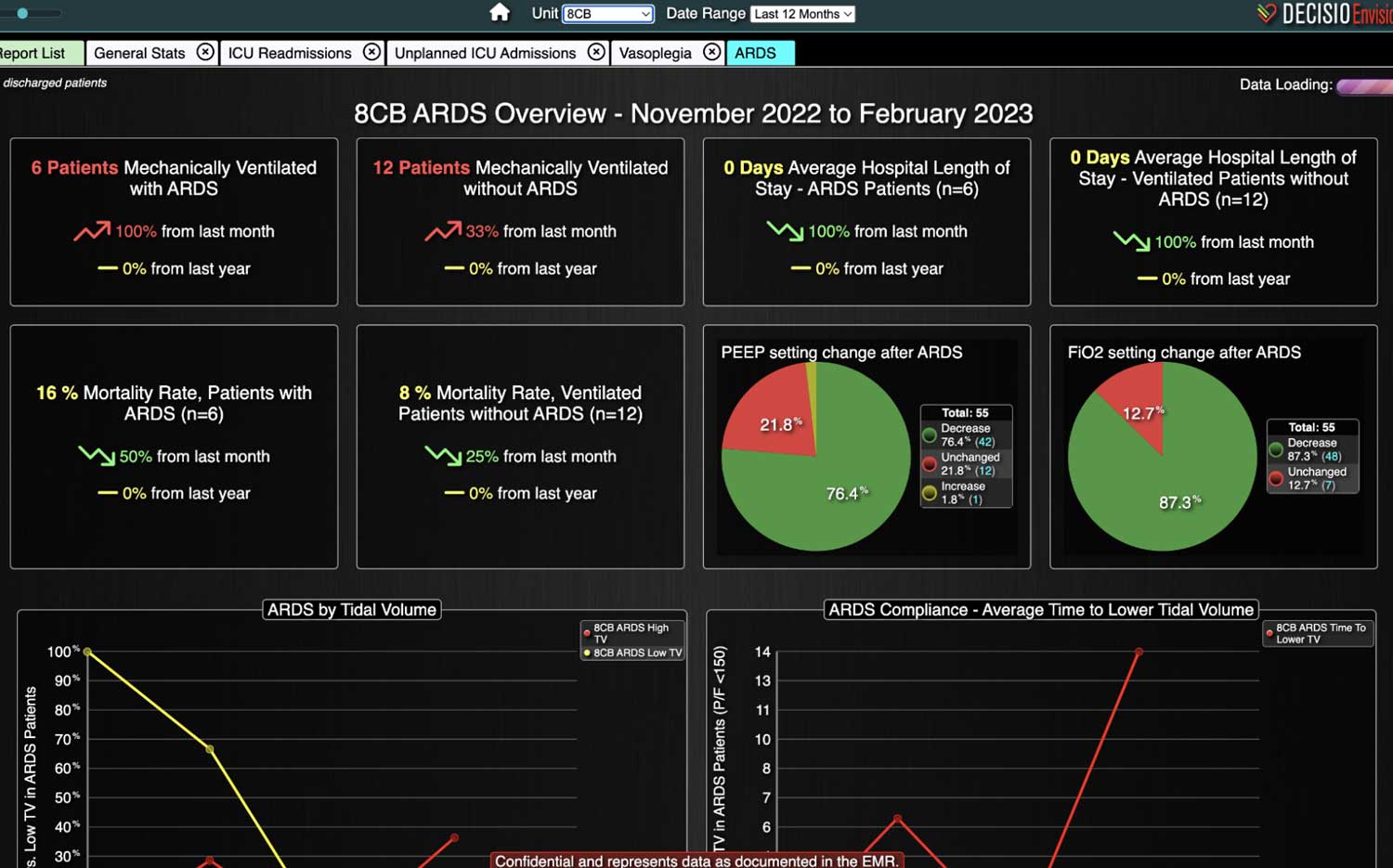
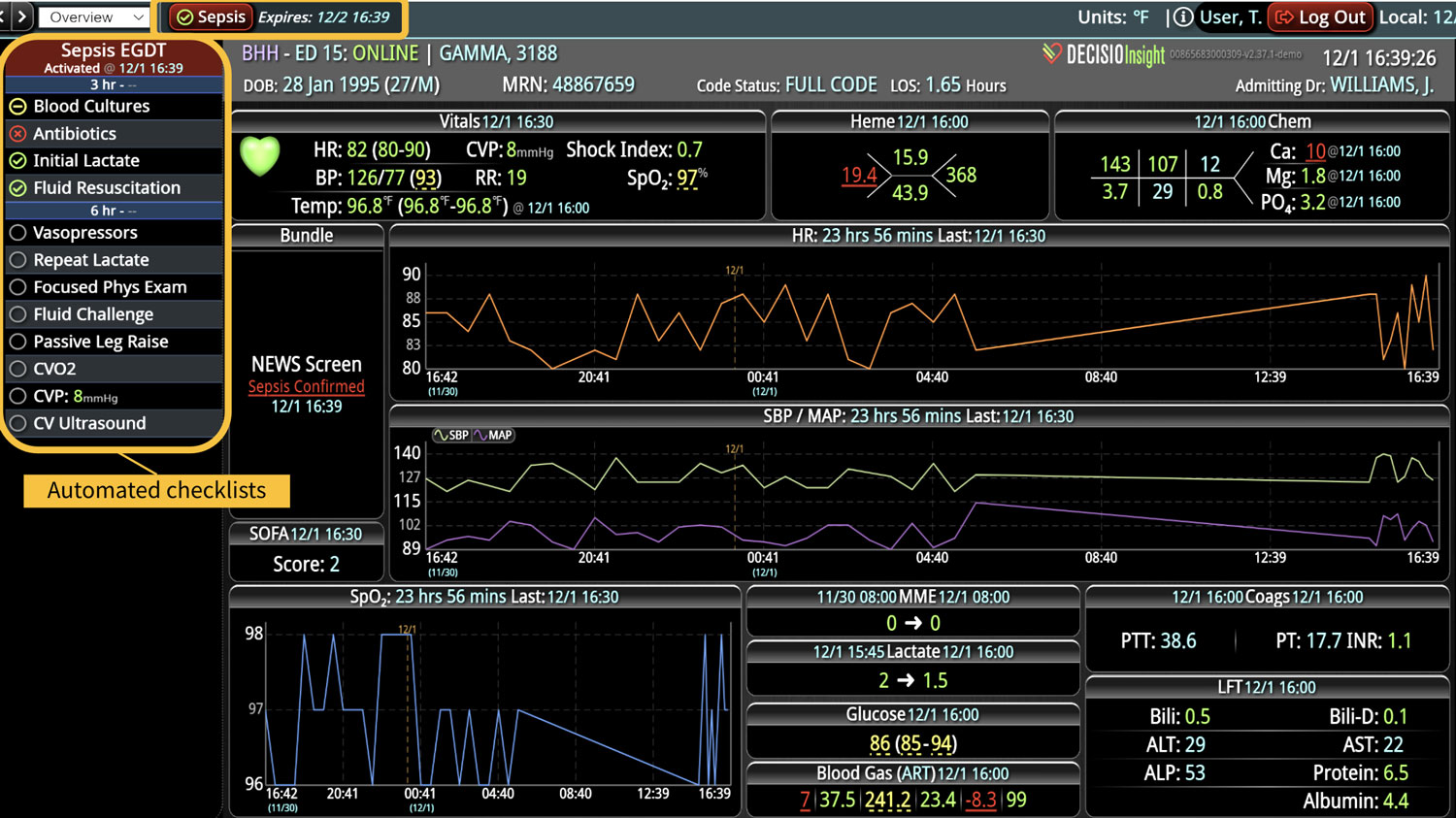
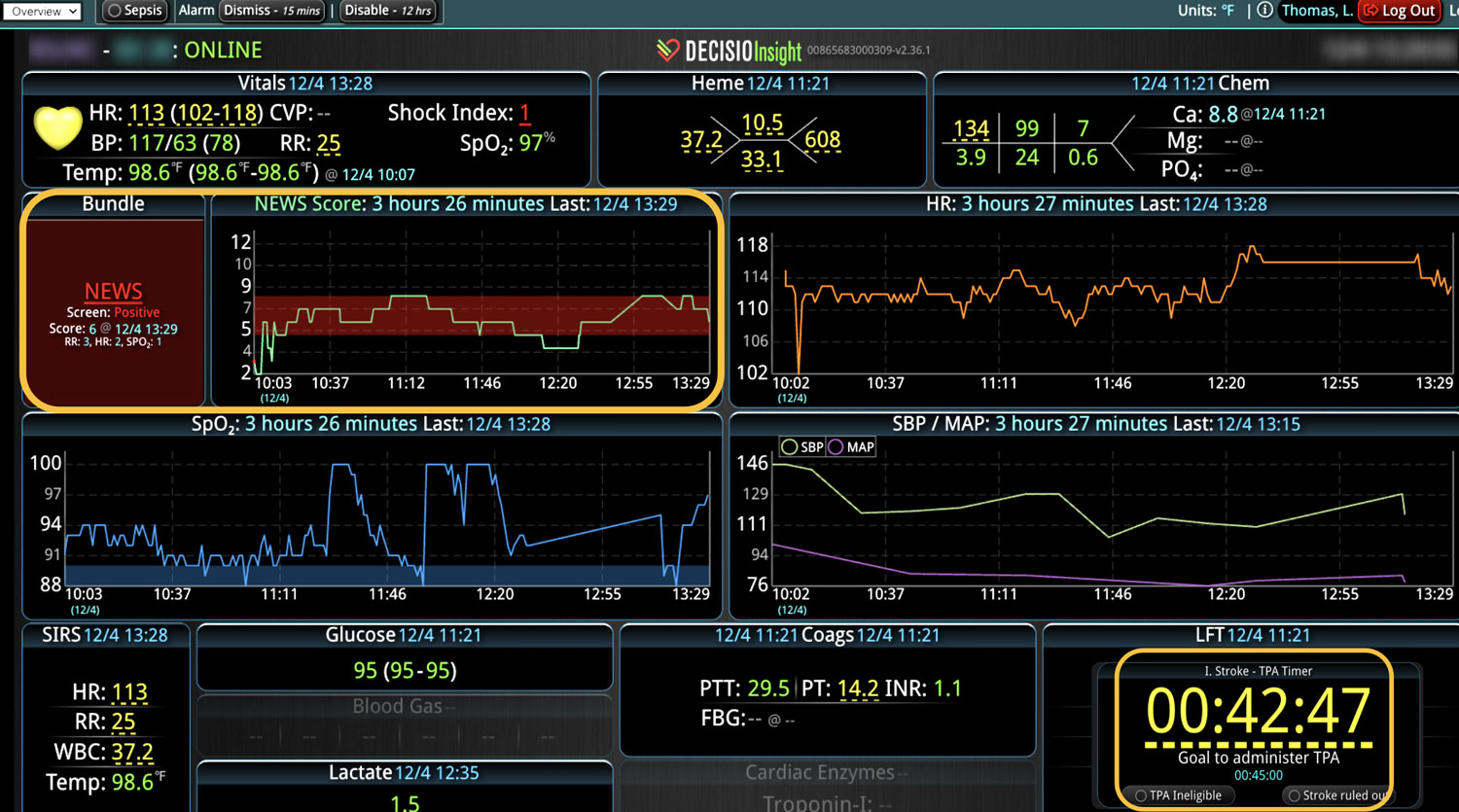
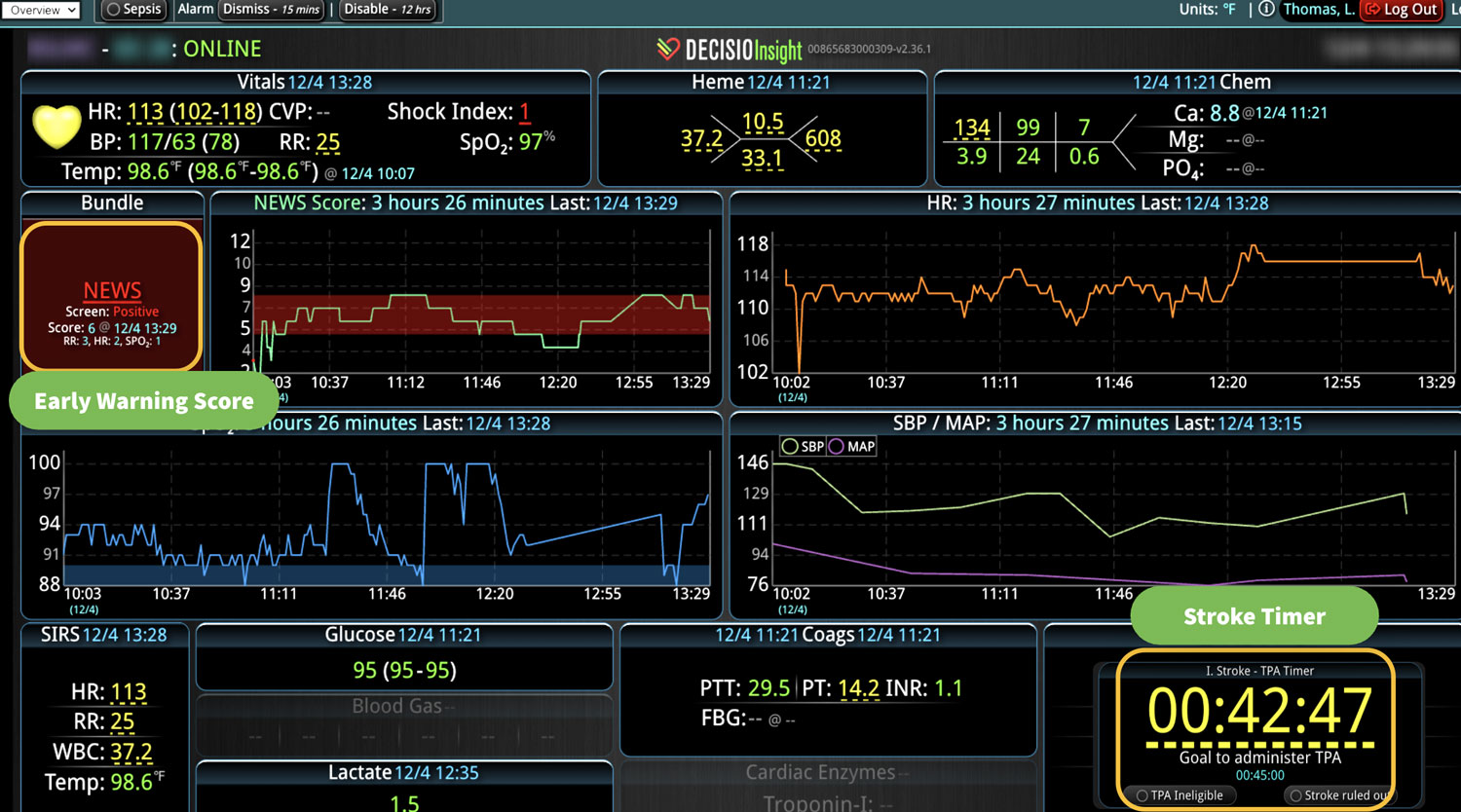
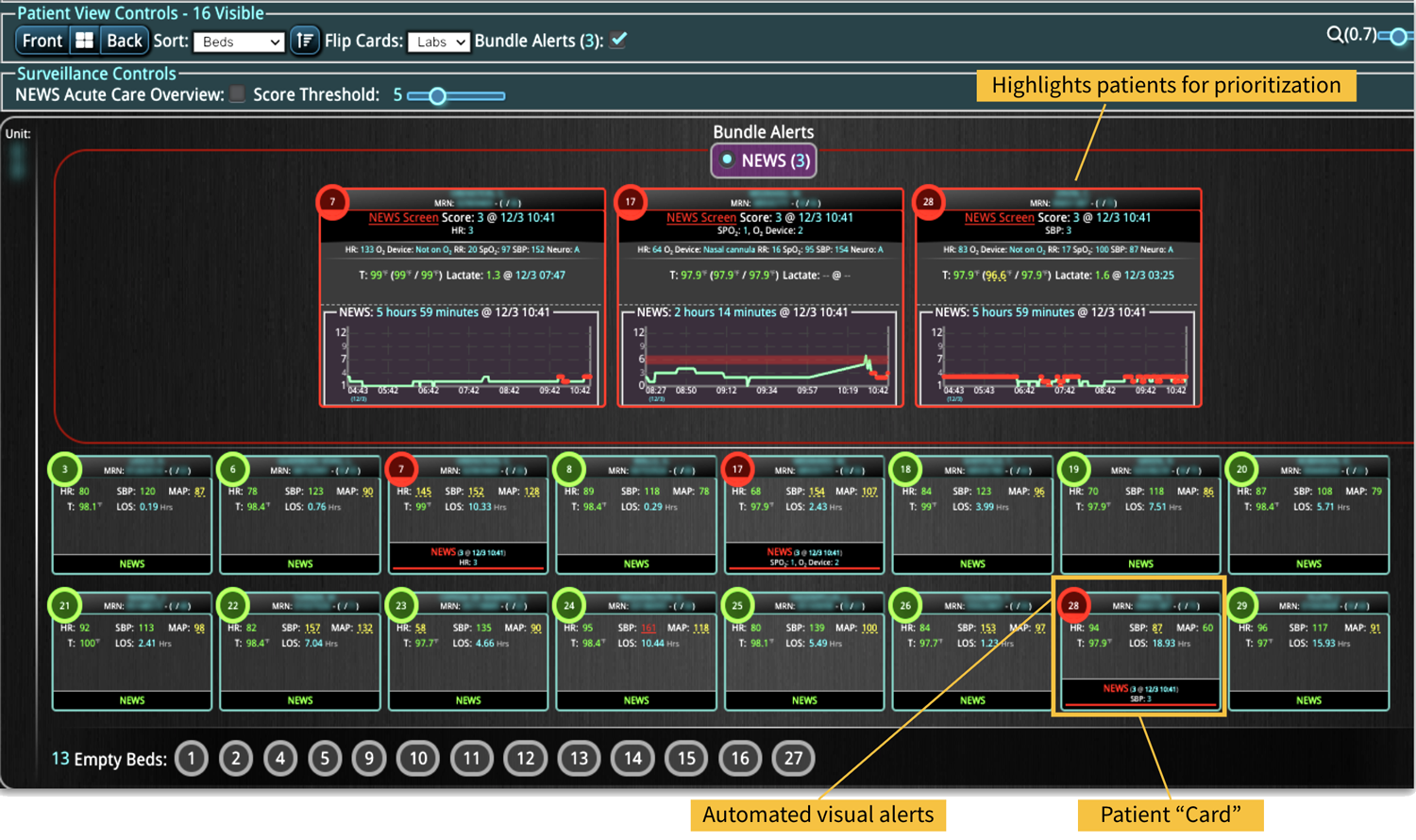
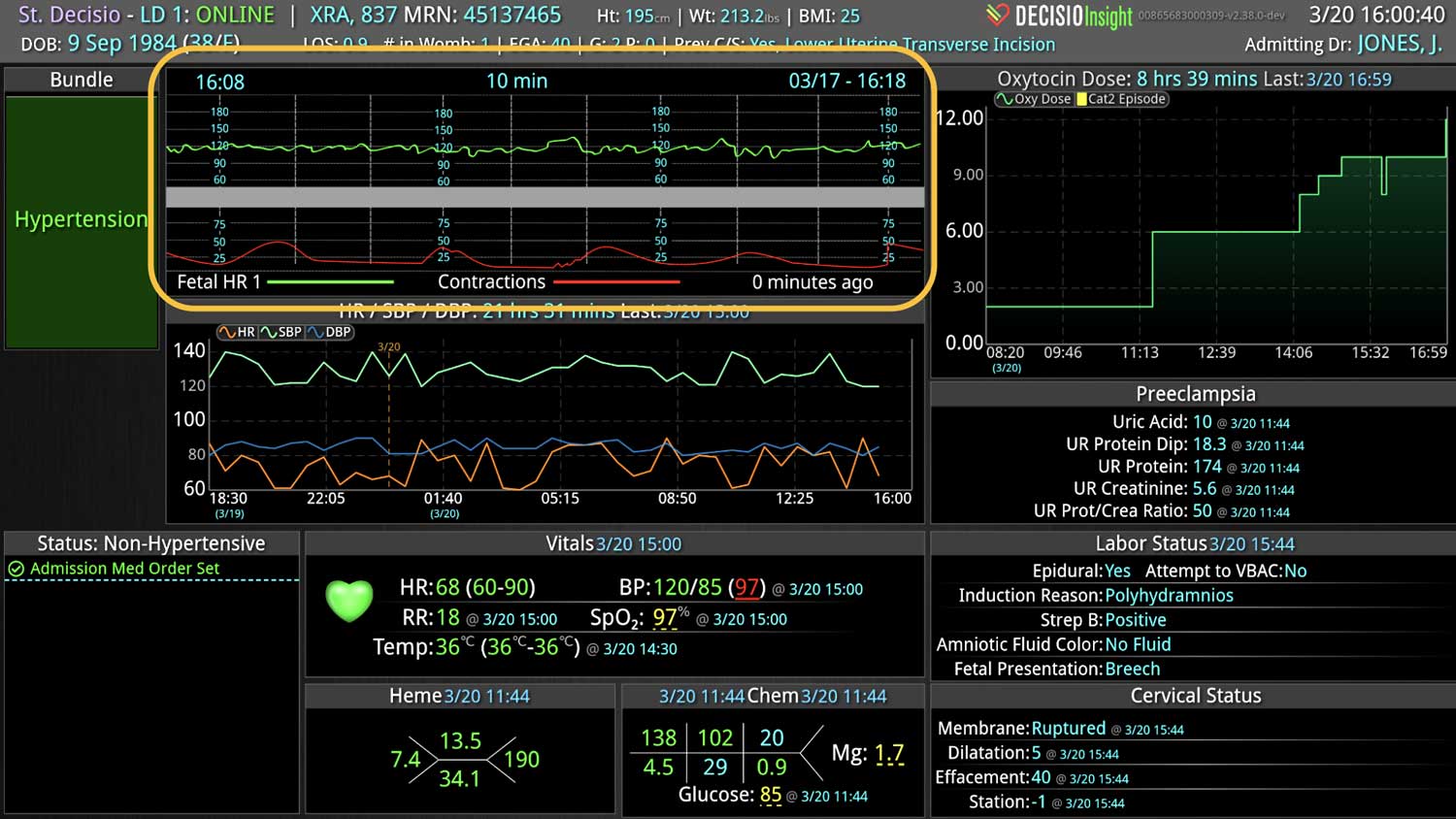
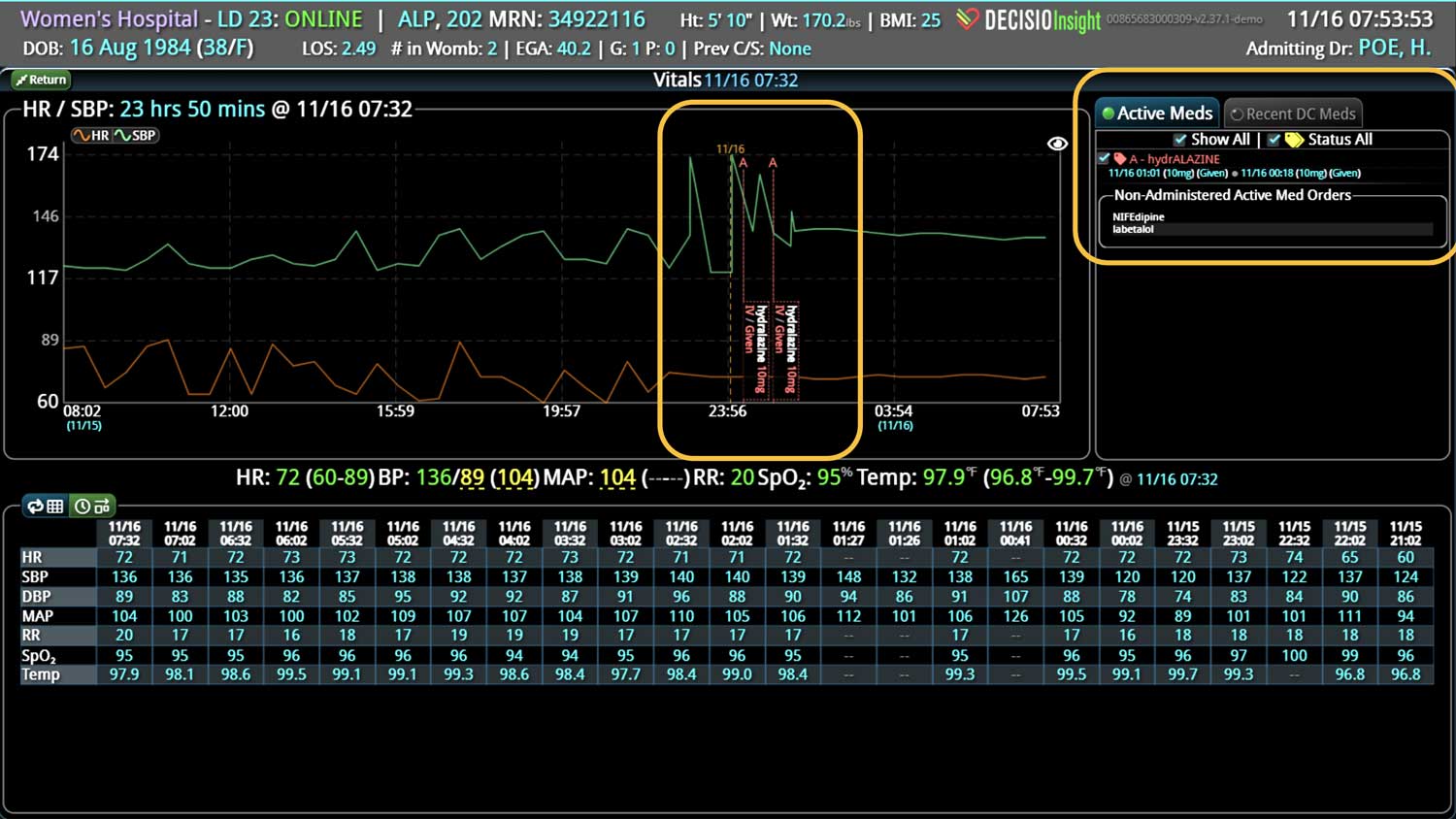
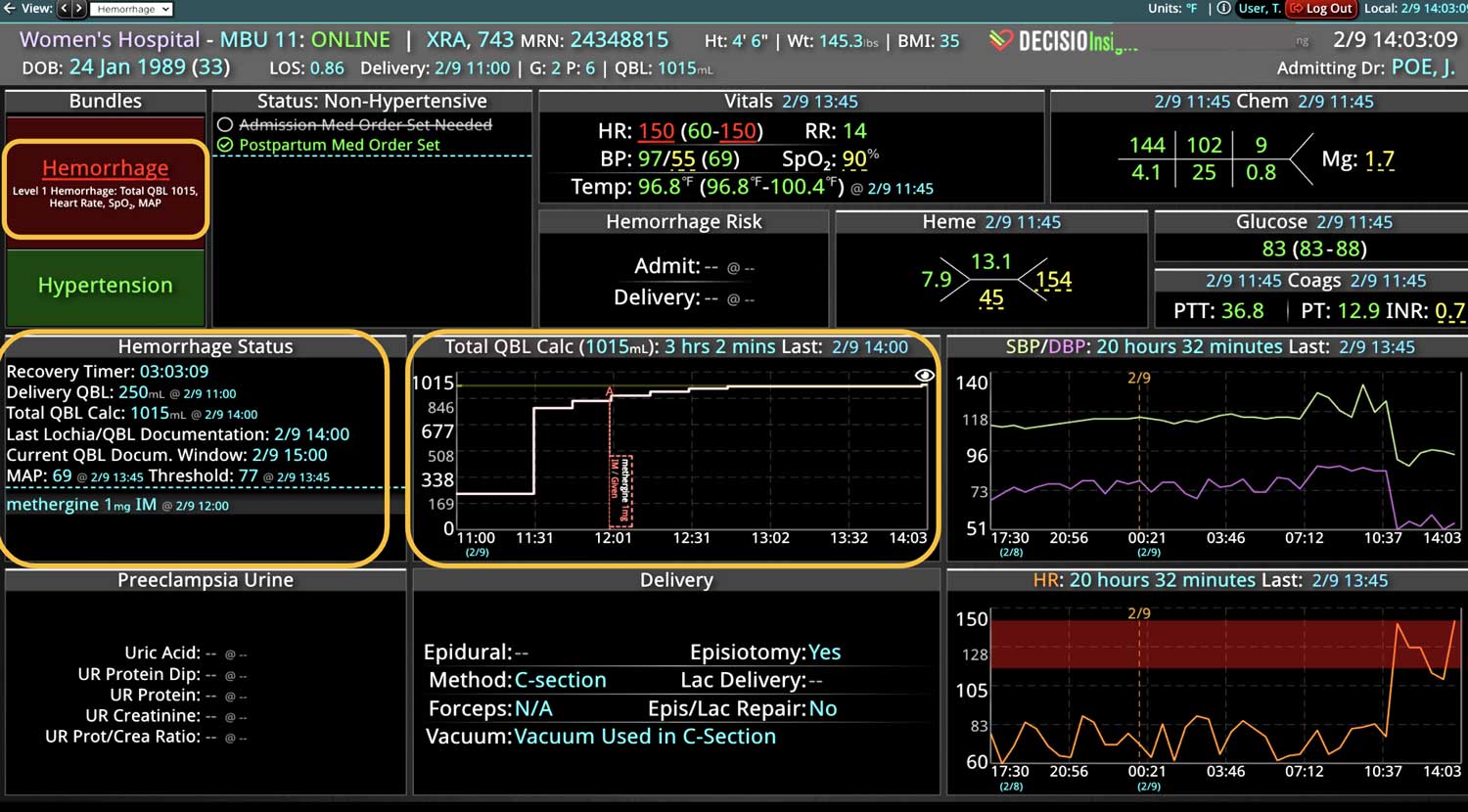
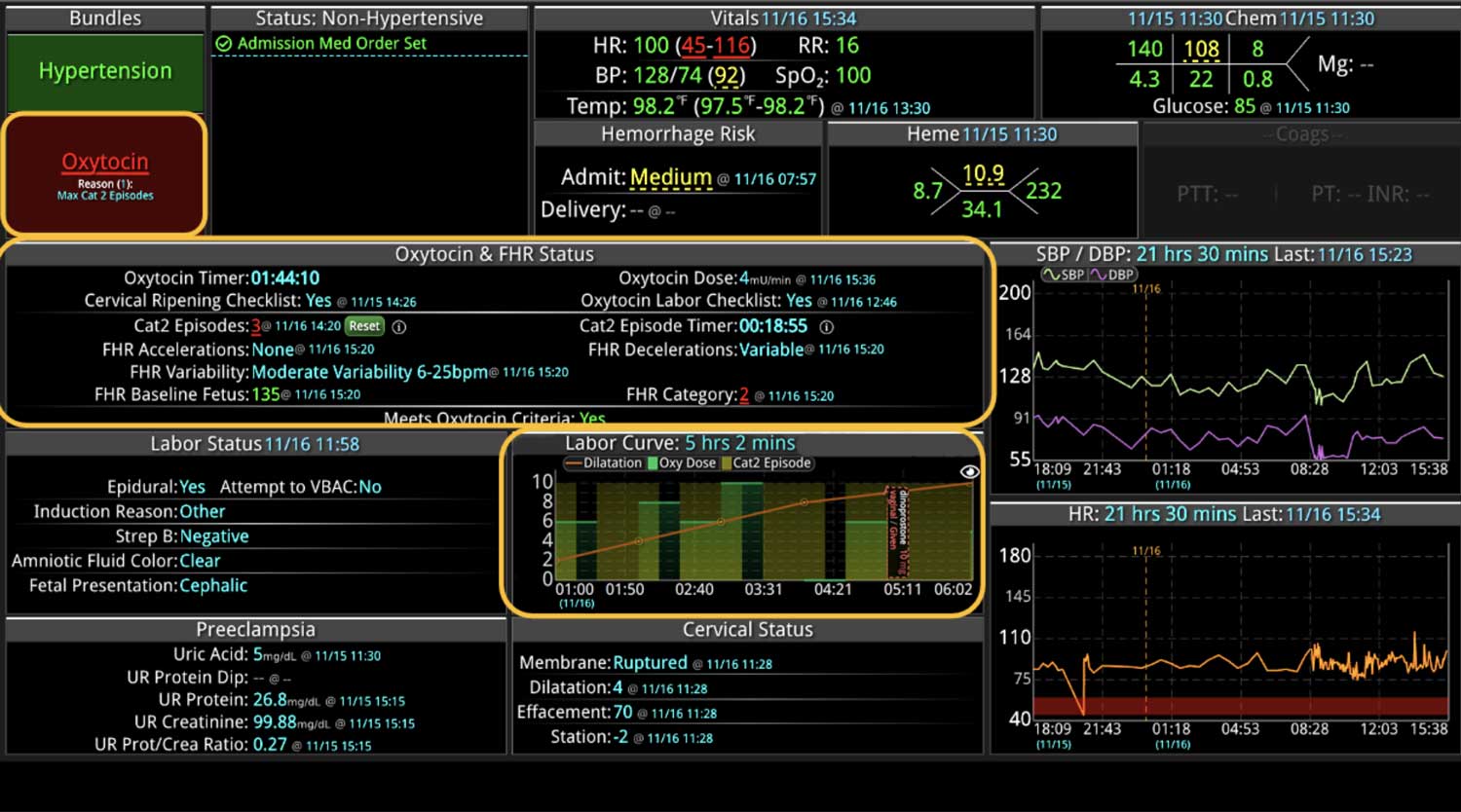
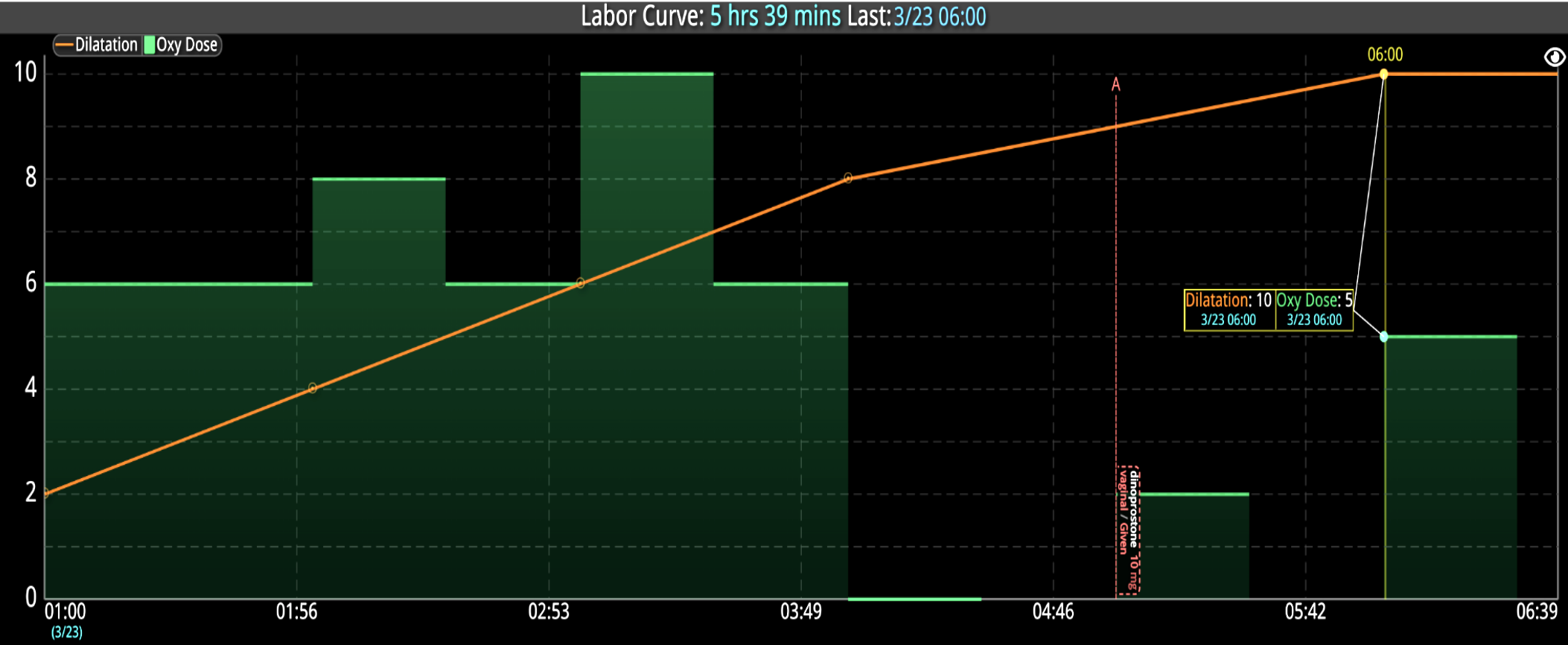
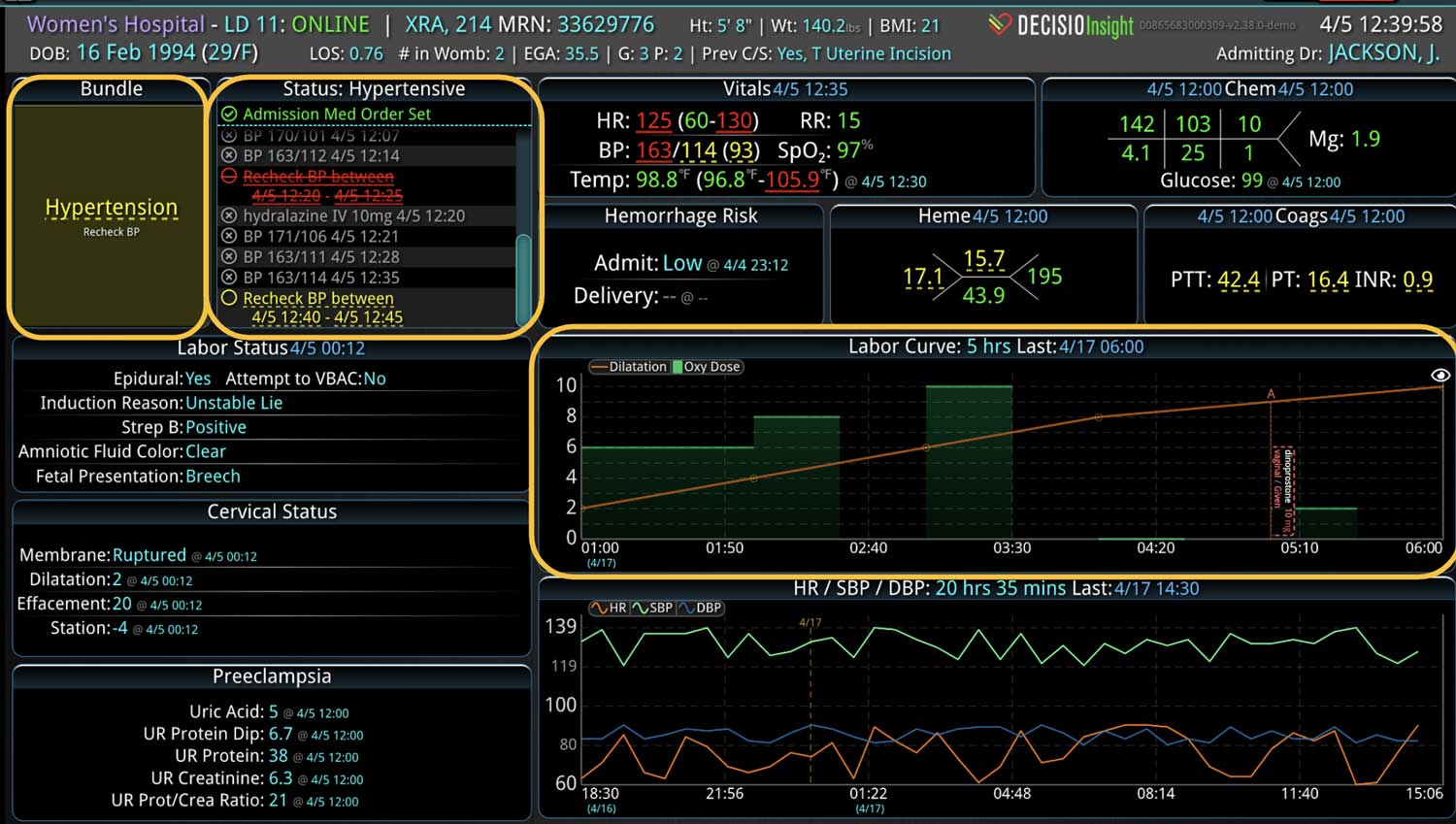
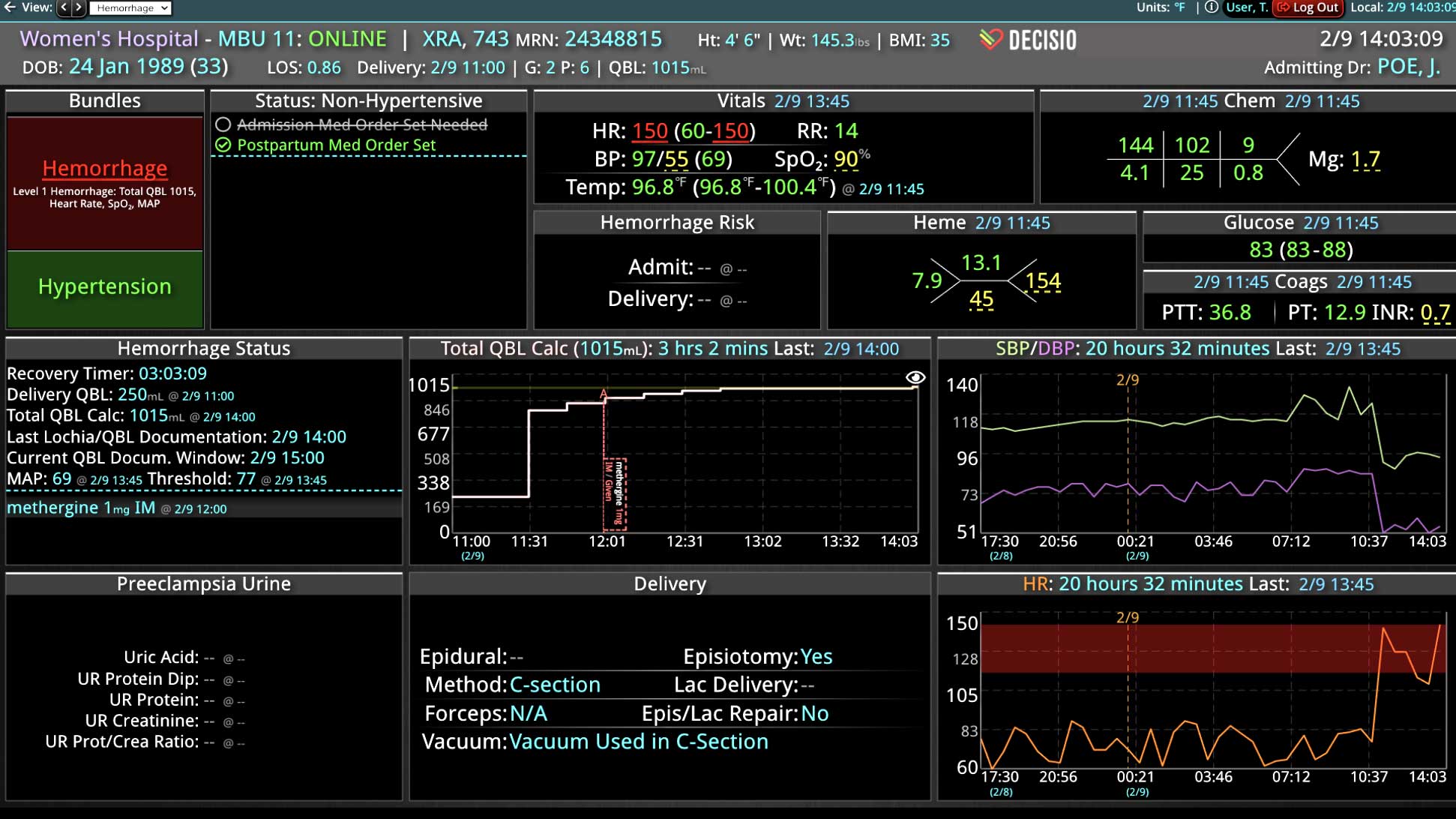
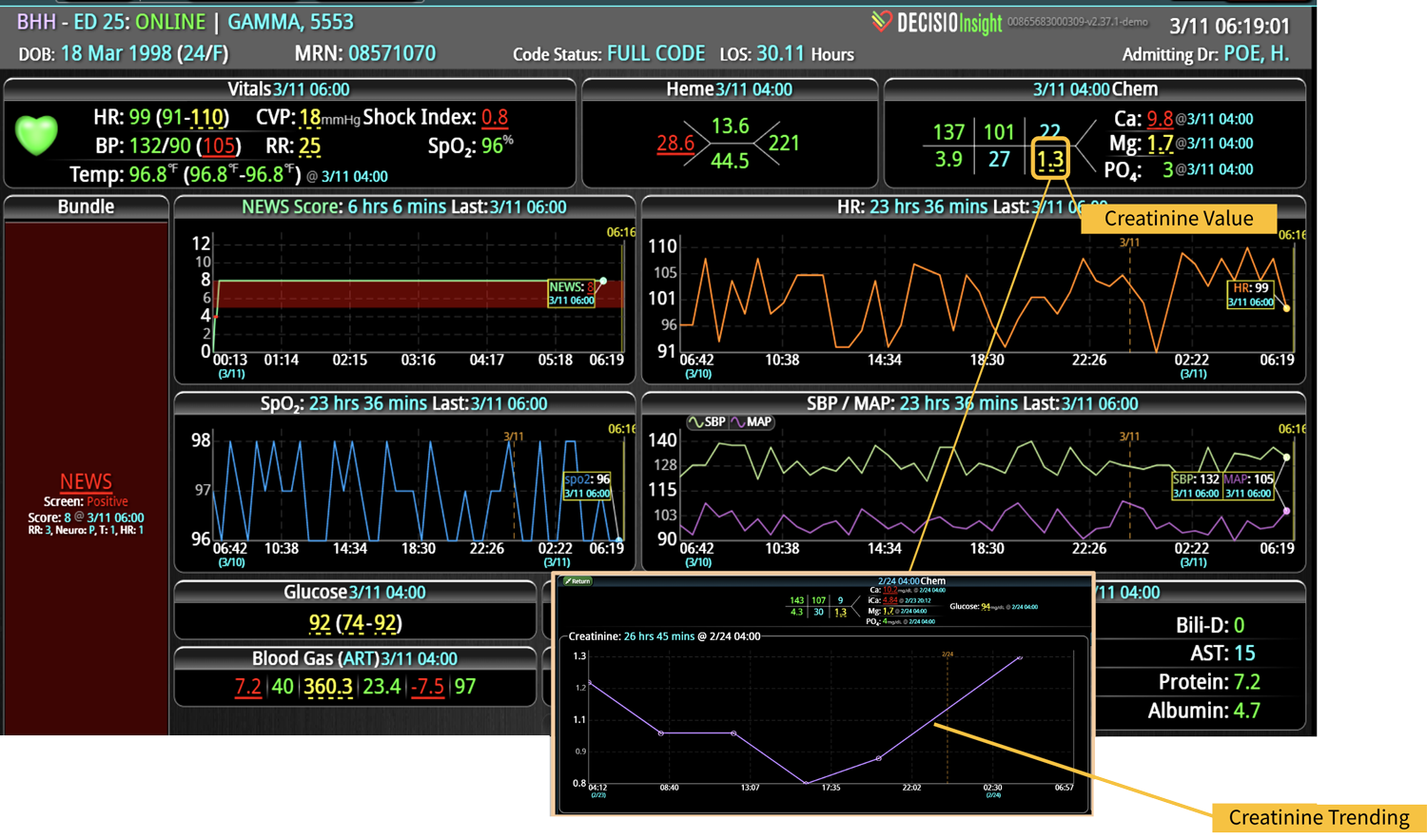
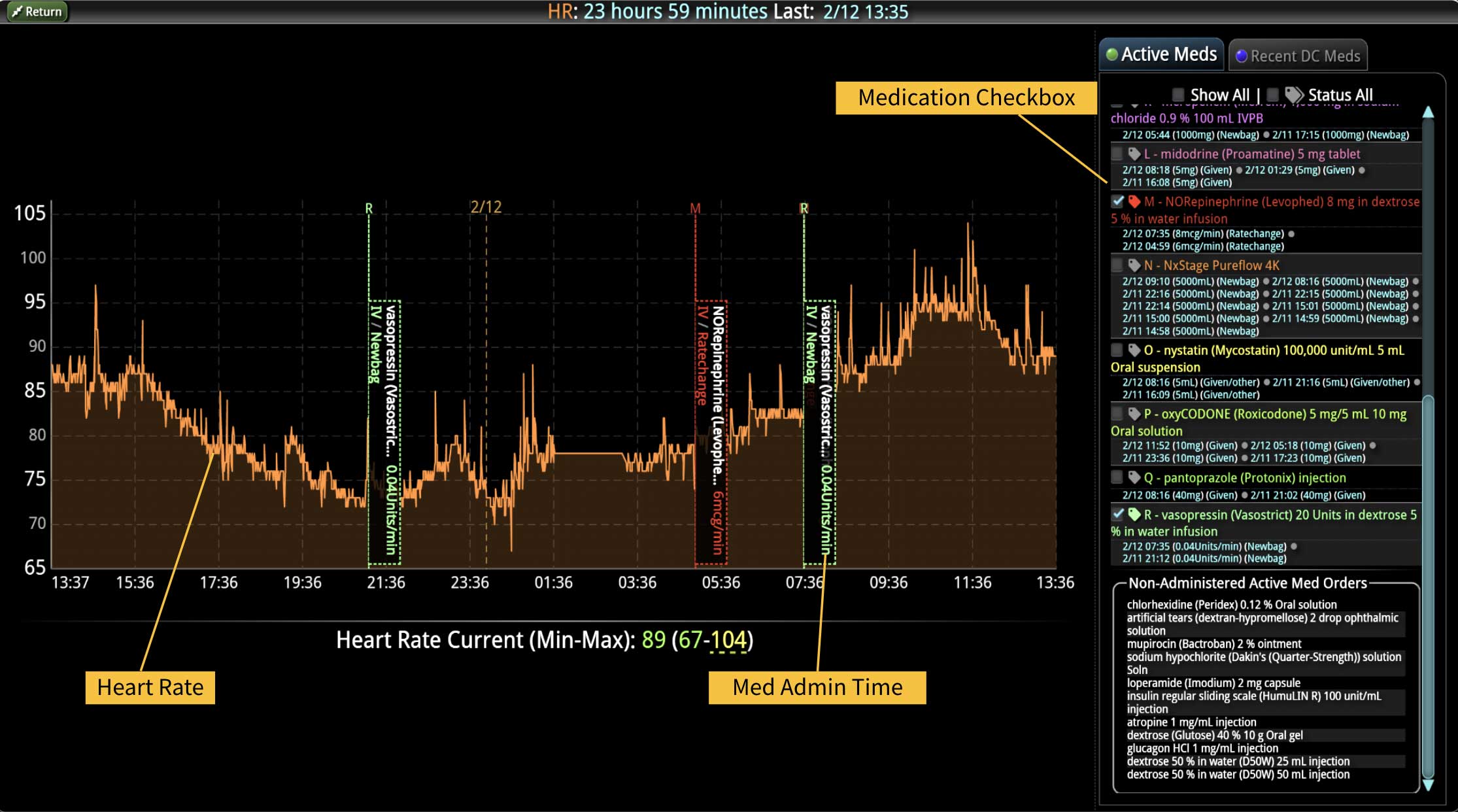
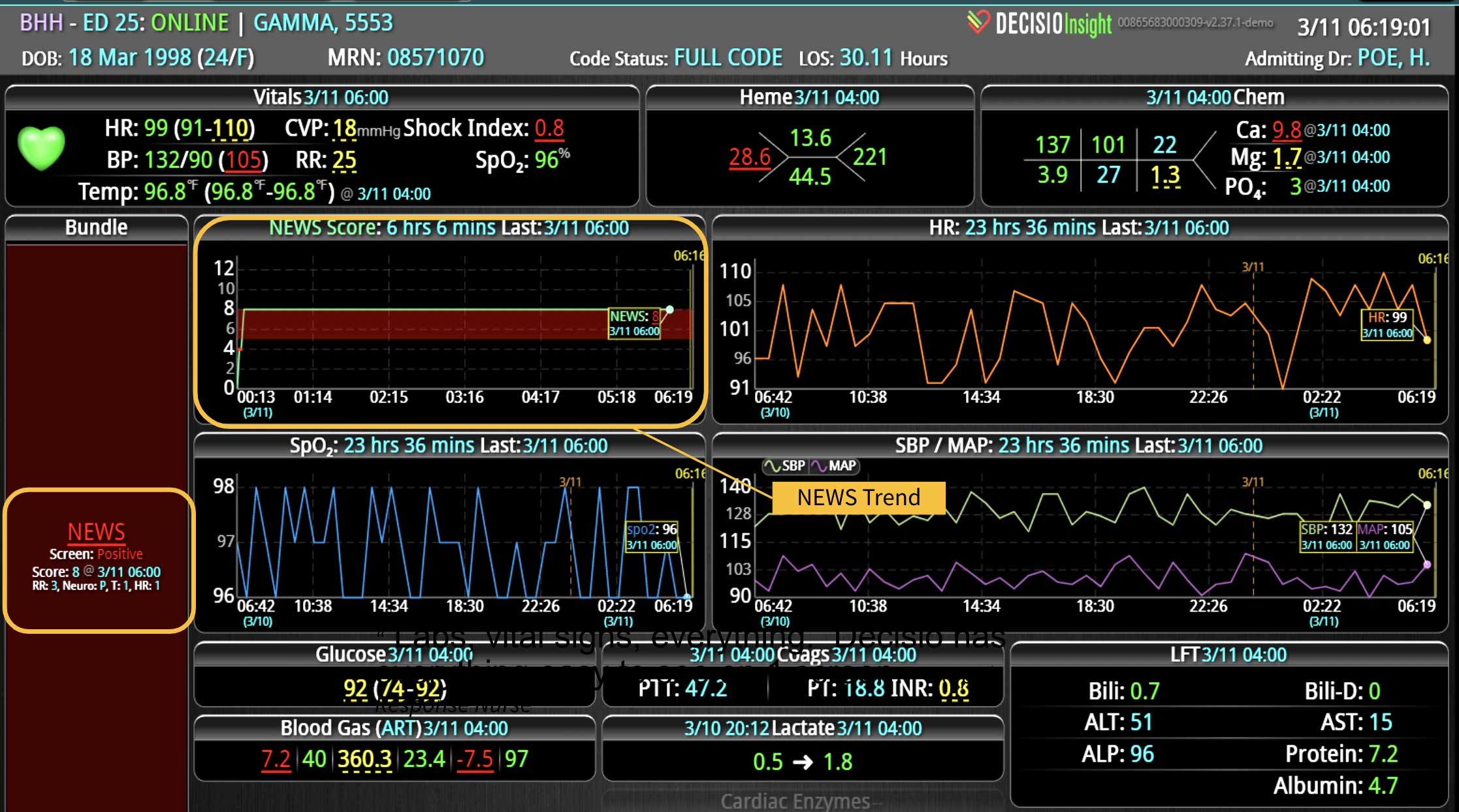
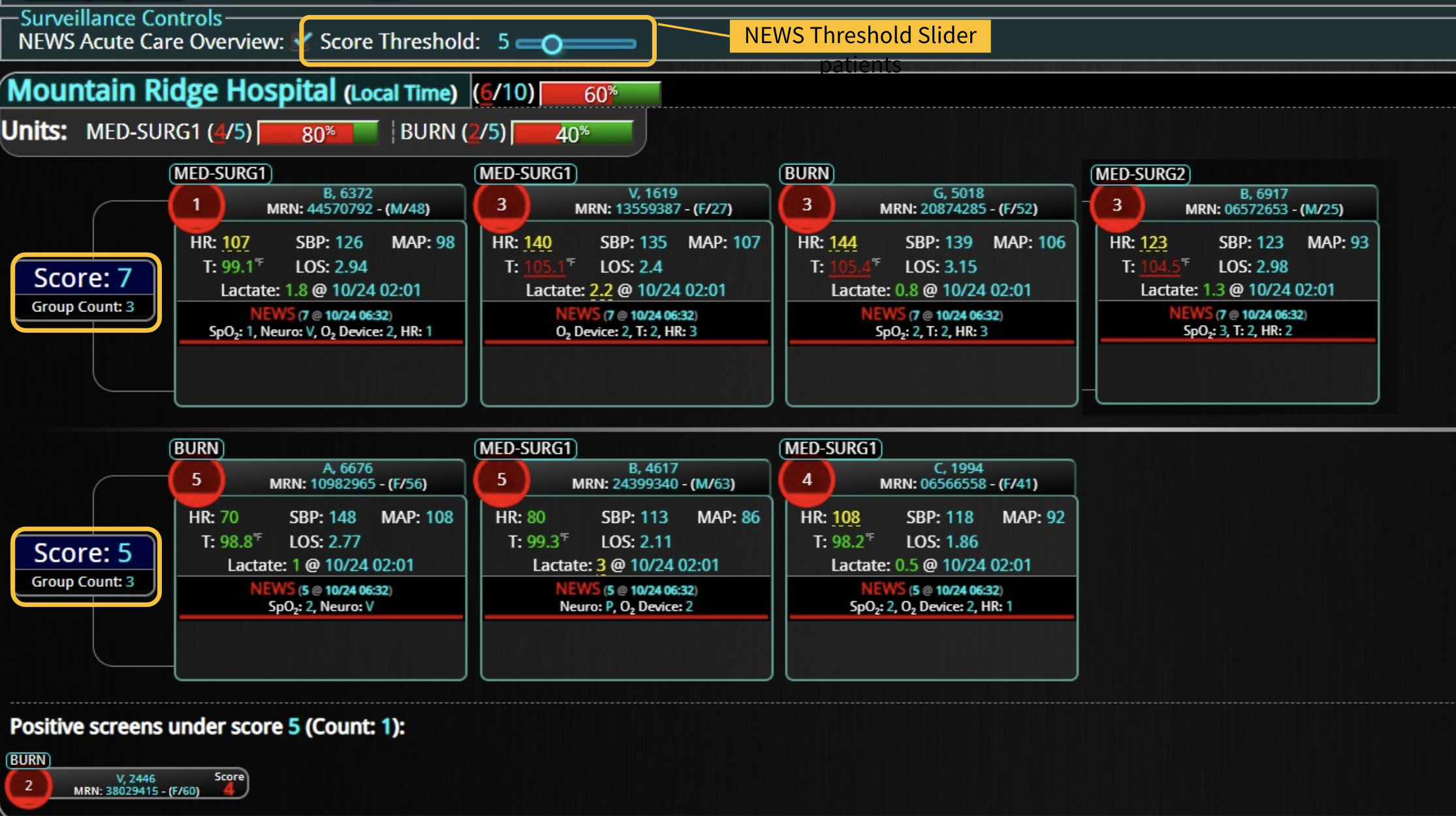
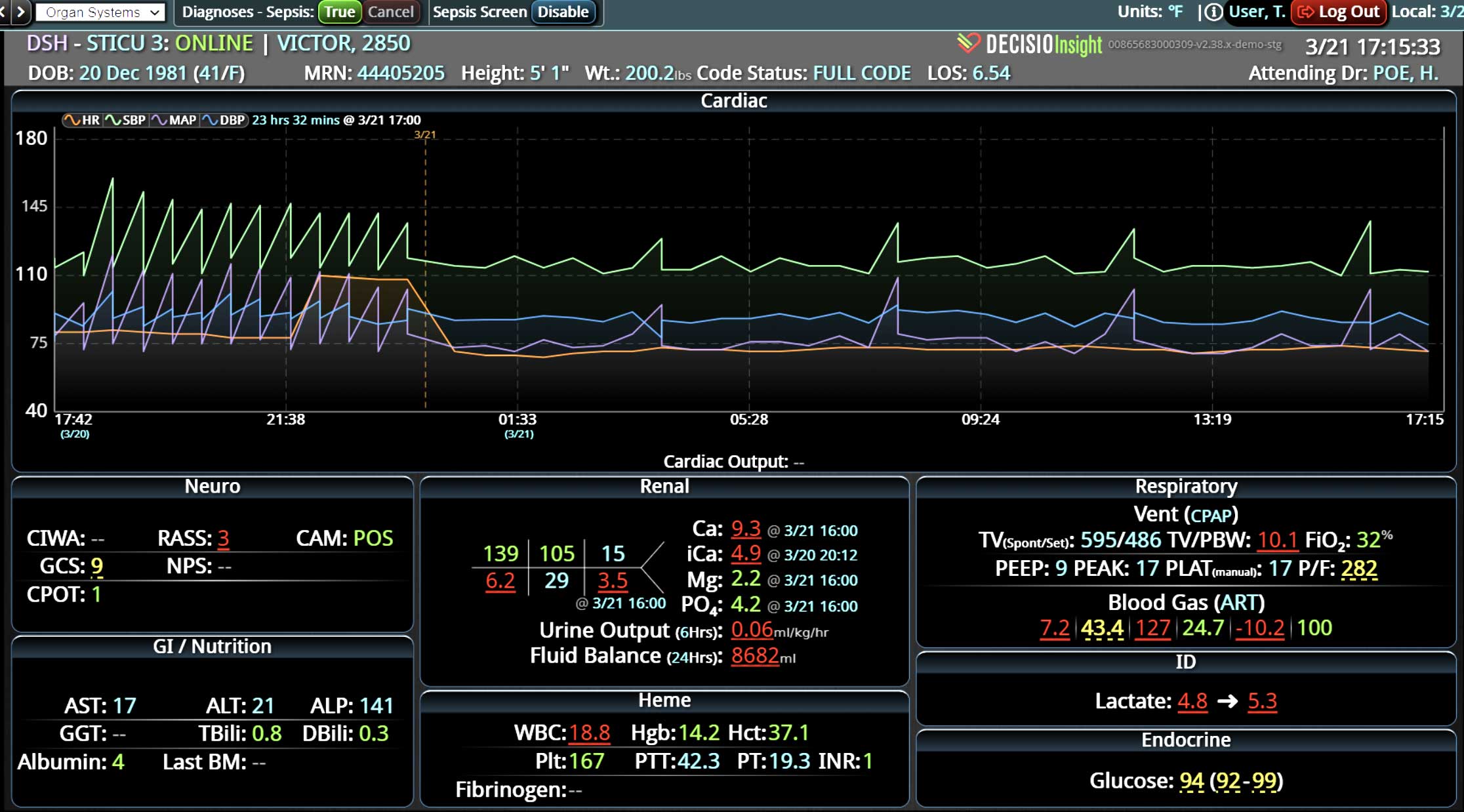
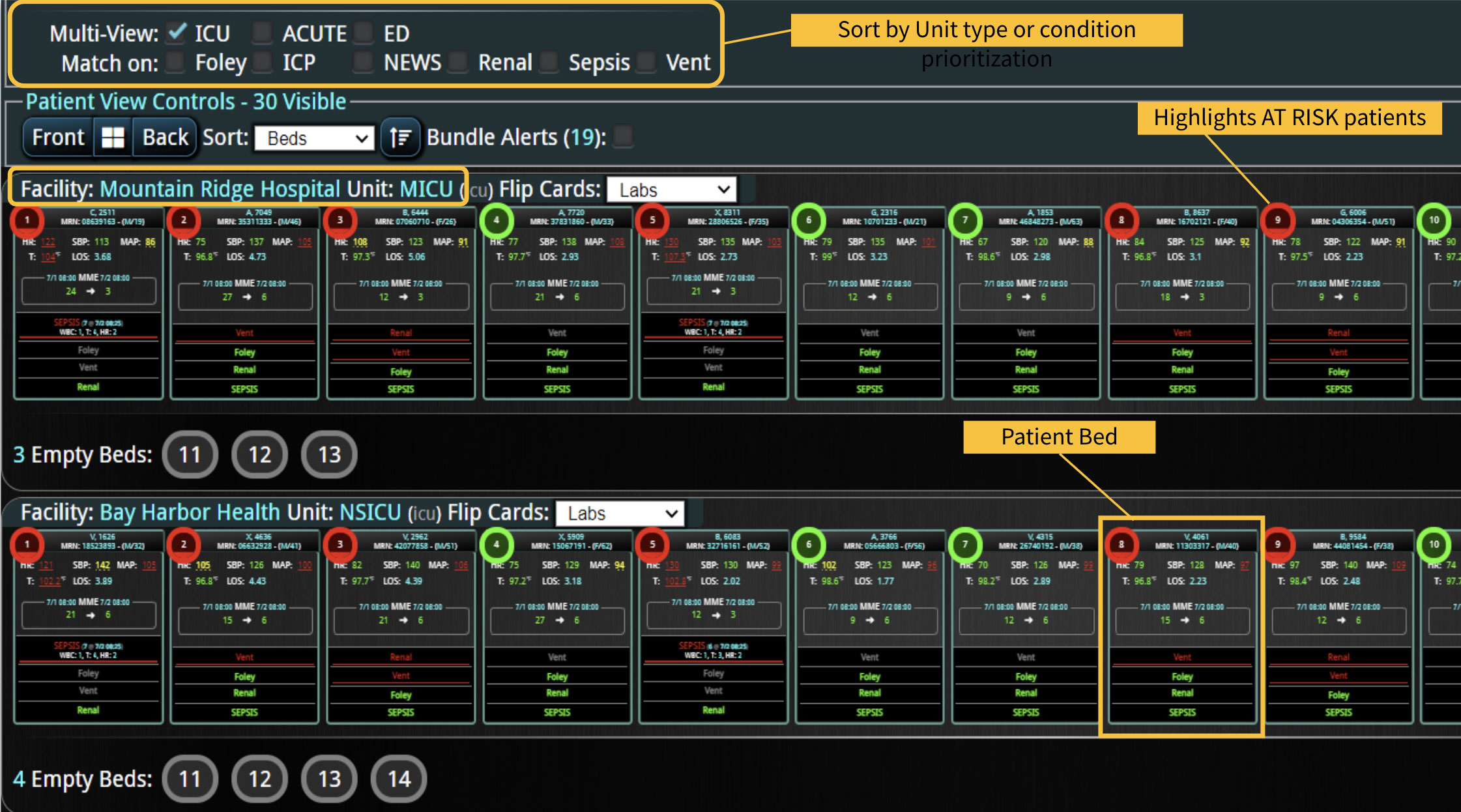
DECISIO is a Texas-based company that has developed InsightIQ, an FDA-cleared, web-native software that uses continuous, smart bedside monitoring that empowers clinical teams to remotely identify at-risk patients and efficiently comply with established clinical guidelines. The InsightIQ software can meet the needs of a wide range of hospital systems and departments to help your team optimize your HaH model. Our software experts work alongside clinicians and administrators to provide a framework for developing unique programs to address specific HaH situations.
Learn more about InsightIQ and DECISIO’s suite of products at: https://www.decisiohealth.com
References
- Klevens RM, Edwards JR, Richards, Jr. CL, et al. Estimating Health Care-Associated Infections and Deaths in U.S. Hospitals. 2002. Pub Health Rec. 2007;122(2): 160-6. https://doi.org/10.1177/003335490712200205
- Shepperd S, Doll H, Angus RM, et al. Avoiding hospital admission through provision of hospital care at home: a systematic review and meta-analysis of individual patient data. CMAJ. 2009 Jan 20;180(2):175-82. http://doi: 10.1503/cmaj.081491
- Hill JD, Hampton JR, Mitchell JRA. A randomised trial of home-versus-hospital management for patients with suspected myocardial infarction. Lancet. 1978 Apr;311(8069):837-41. https://doi.org/10.1016/S0140-6736(78)90190-3
- Hostetter M, Klein S. Has the time come for hospital at home? Transforming Care. The Commonwealth Fund. Published 2020 July 7. Accessed October 30, 2022. Available from: https://www.commonwealthfund.org/publications/2020/jul/has-time-finally-come-hospital-home
- CMS News and Media Group. CMS announces comprehensive strategy to enhance hospital capacity amid COVID-19 Surge. Published 2020 Nov 25. Available from: https://www.cms.gov/newsroom/press-releases/cms-announces-comprehensive-strategy-enhance-hospital-capacity-amid-covid-19-surge
- Acute Hospital Care at Home Resources. CMS.gov [Website]. Updated 2022 Nov 15. Available from: https://qualitynet.cms.gov/acute-hospital-care-at-home/resources
- Wicklund E. Kaiser Permanente, Mayo launch coalition to support home-based telehealth, RPM. Telehealth News. Published 2021 Oct 14. Available from: https://mhealthintelligence.com/news/kaiser-permanente-mayo-launch-coalition-to-support-home-based-telehealth-rpm
- Weiner S. Interest in hospital-at-home programs explodes during COVID-19. AAMC News. Published 2020 Sept 29. Available from: https://www.aamc.org/news-insights/interest-hospital-home-programs-explodes-during-covid-19
Learn more About How we help clinicians improve patient outcomes
Schedule a call with our team to discuss how we are helping our clients revolutionize how clinicians manage patient interventions.