25 Jul Prioritizing Quality of Patient Care: A Culture Shift in Hospitals
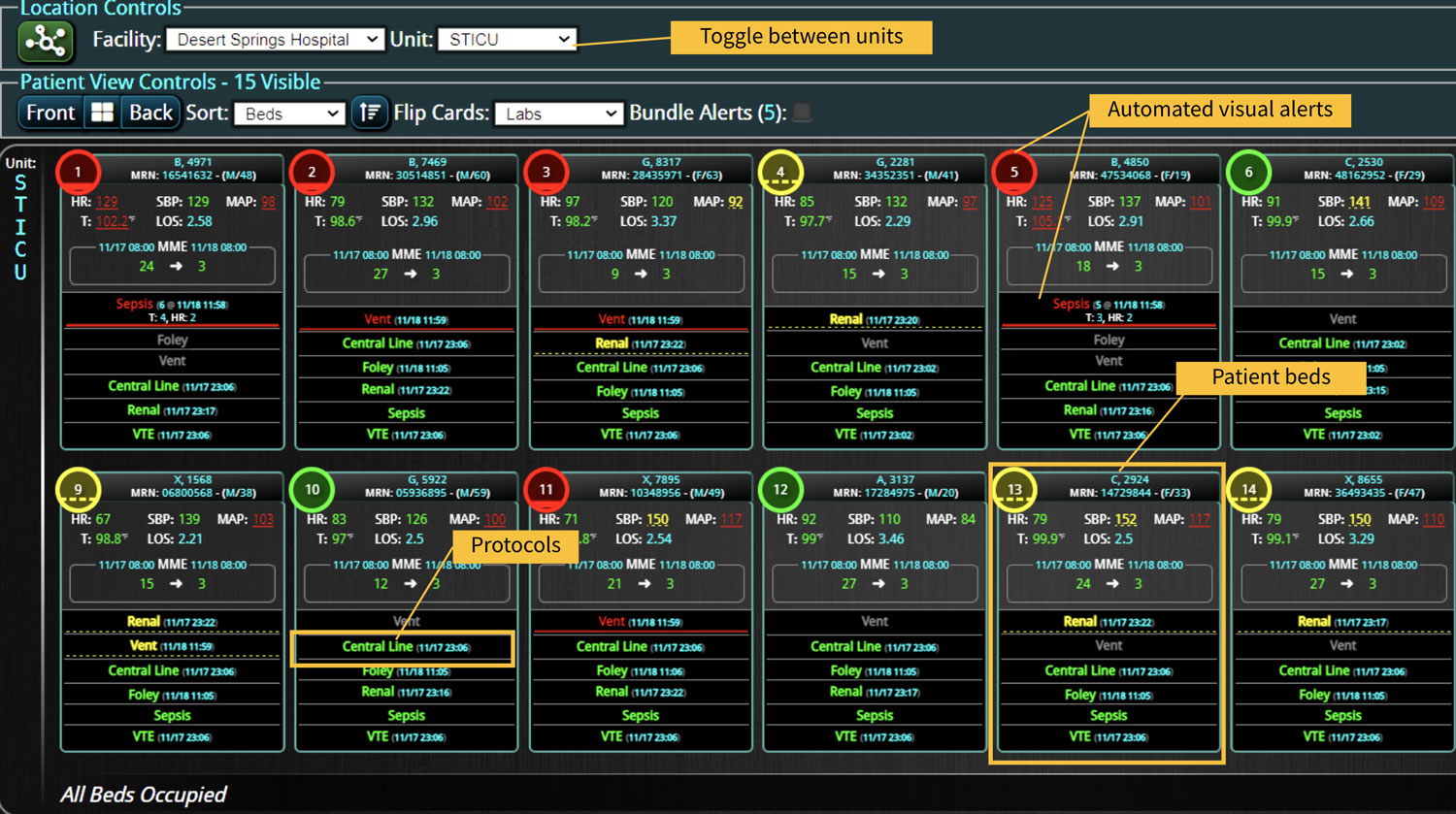
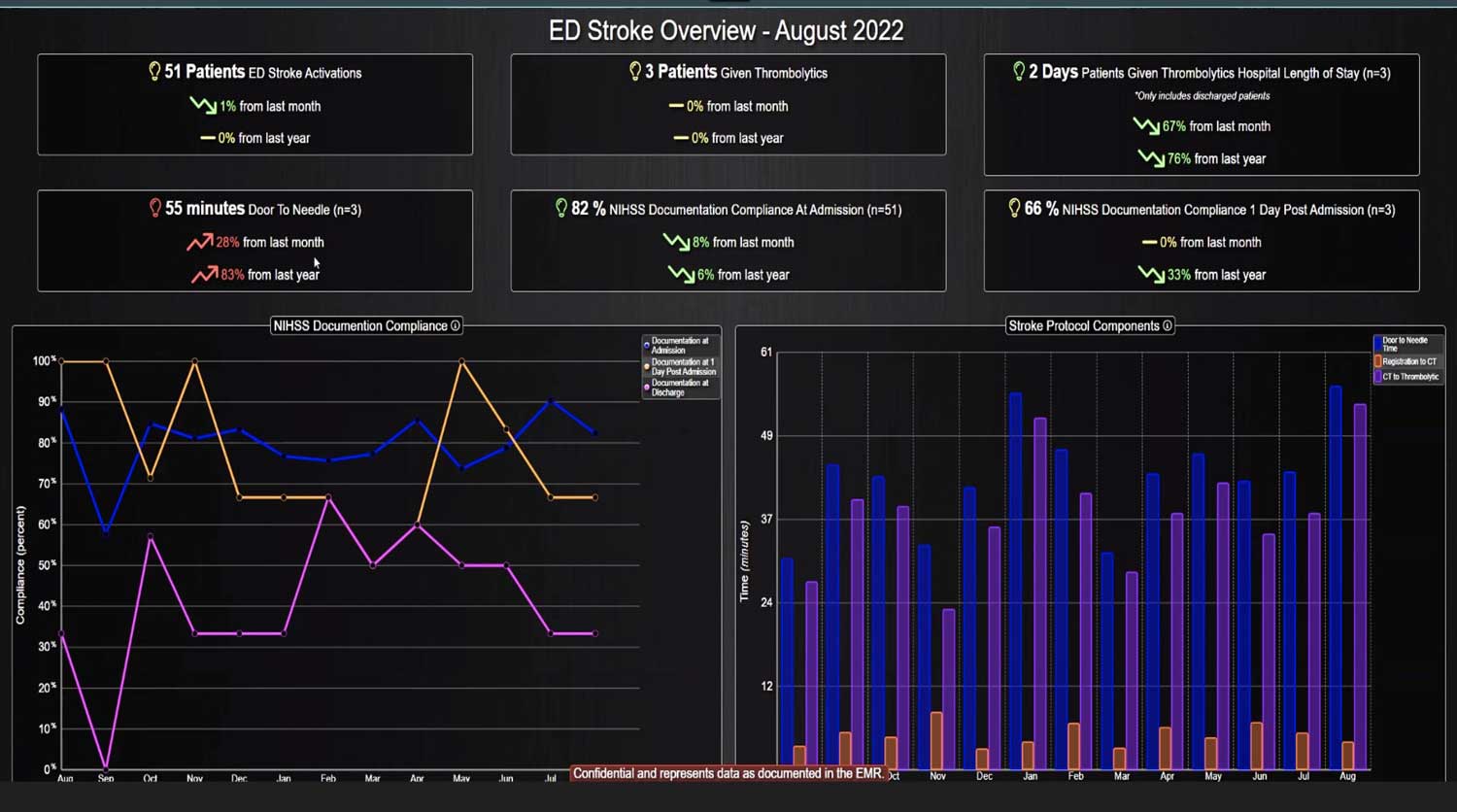
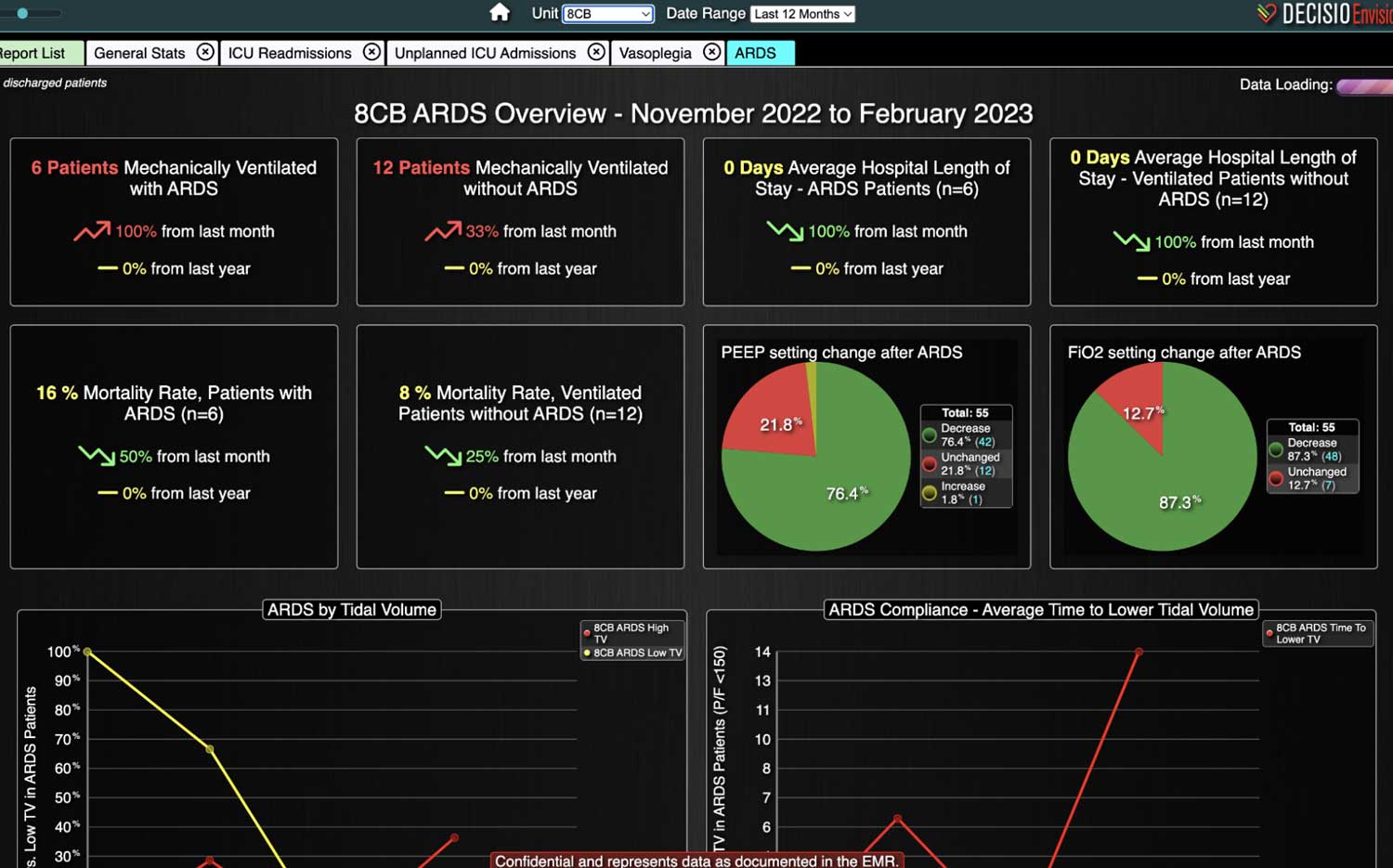
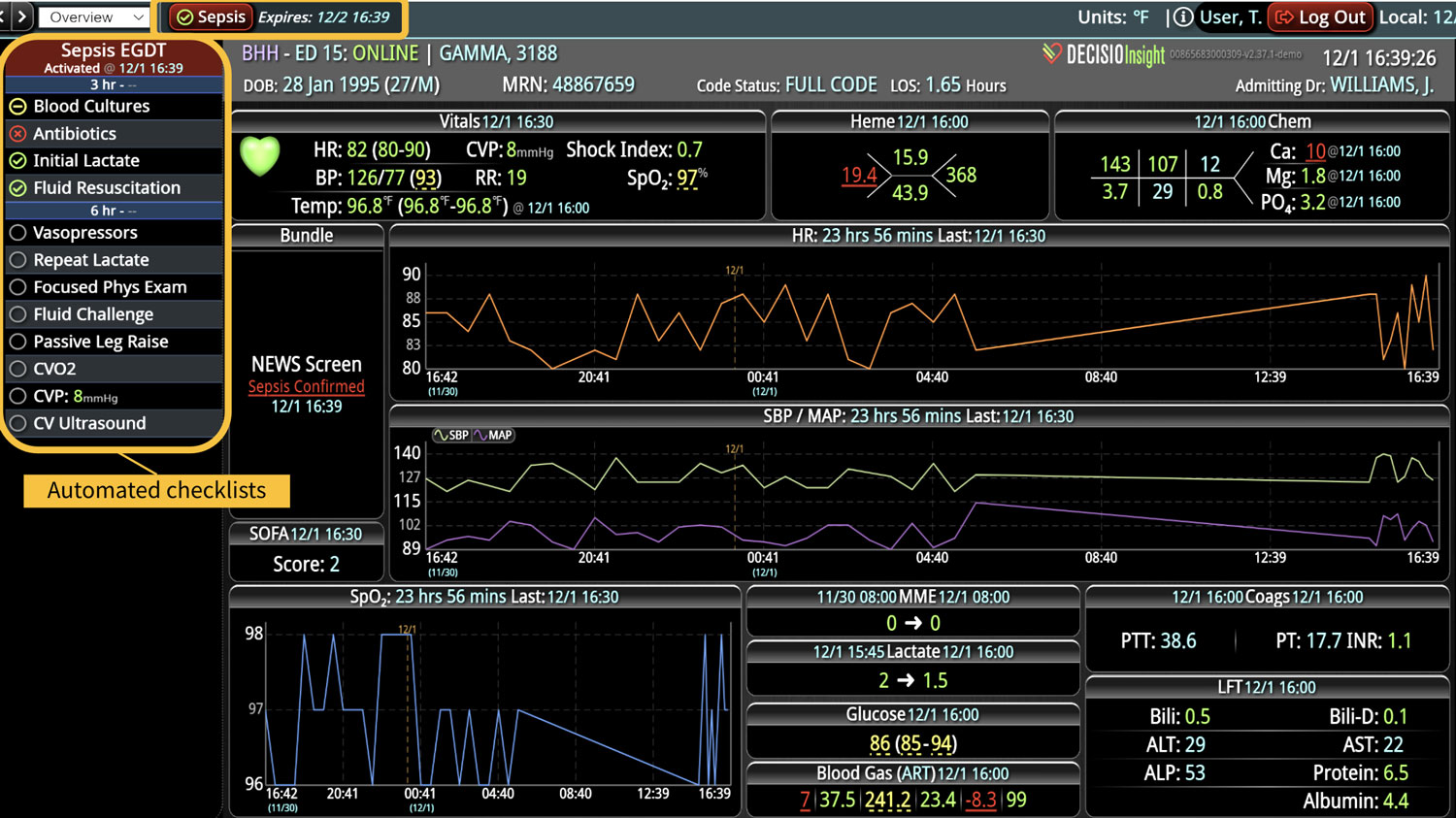
Transforming a hospital to prioritize the improvement to the quality of patient care they deliver requires a comprehensive cultural shift. This change requires cultivating a mindset dedicated to continuous improvement and better patient outcomes, extending far beyond merely adopting new software and tools. Below we will review strategies hospitals can incorporate to help achieve this transformation, as well as the benefits once they do. The Importance of Quality of Care Prioritizing superior patient care is the cornerstone of top healthcare systems. Improving patient care leads to better clinical outcomes, increased patient satisfaction, and reduced healthcare costs. According to the Agency for Healthcare Research and Quality (AHRQ), hospitals that prioritize quality care experience fewer medical errors and higher patient satisfaction rates. Steps to Shift the Cultural Mindset 1. Leadership Commitment The commitment to quality must start at the top. Hospital leaders should articulate a clear vision for quality care and model the behaviors they want to see in their staff. Communicating that quality care is a top priority and backing this up with resources and support is the best goal for a leadership team. 2. Engaging and Empowering Staff Engagement and empowerment of all staff levels are crucial. Frontline healthcare workers should be involved in decision-making processes and...